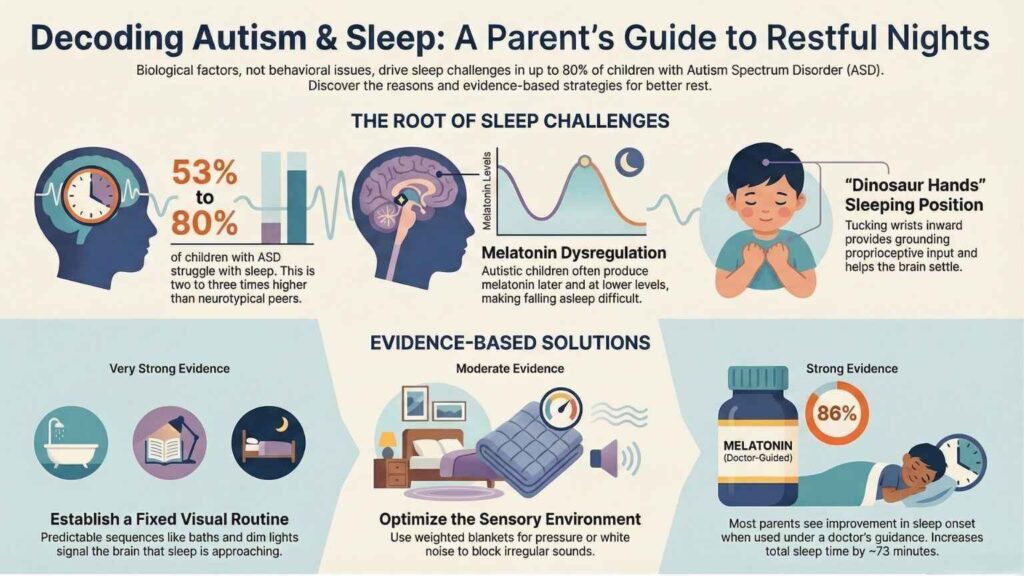
If your child with autism struggles to fall asleep, wakes up repeatedly at night, or sleeps curled up in unusual positions you are not alone. Sleep problems affect 53% to 80% of children with autism spectrum disorder (ASD), a rate two to three times higher than in typically developing children. [1] This guide explains why autistic children sleep differently, what those unique sleeping positions mean, and what you can actually do to help.
Why Do Children with Autism Sleep Differently?
Autism affects the brain’s development in ways that directly impact sleep. It is not a parenting issue or a discipline problem. There are real biological and neurological reasons behind the sleep challenges your child is experiencing. Understanding them is the first step to helping.
Melatonin dysregulation is one of the biggest culprits. Research shows that many children with ASD produce melatonin later and at lower levels than neurotypical children. [2] Melatonin is the hormone that tells the brain it is nighttime and time to sleep. When it is delayed or reduced, falling asleep becomes genuinely difficult, not a choice.
Sensory sensitivities also play a major role. Sheets that feel scratchy, sounds that seem faint to others, or the pressure of a blanket can all trigger discomfort that keeps a child wide awake. Many autistic children also have heightened anxiety at bedtime, especially around changes in routine, which activates their nervous system instead of calming it.
Read More: Strategies for Coping With Disruptive Behavior: Evidence-Based ABA Techniques
Common biological reasons for autism sleep problems include:
- Melatonin pathway abnormalities: disrupted circadian rhythm and delayed sleep onset [3]
- Sensory processing differences: sensitivity to light, sound, touch, and temperature
- Anxiety and hyperarousal: difficulty transitioning from an activated state to rest
- Gastrointestinal issues: common in ASD and known to disrupt nighttime sleep
- Medication side effects: some ASD-related medications can interfere with sleep architecture
Your Child's Sleep Affects Everything - Behavior, Learning & Growth.
Fill in the form below to discuss how your child could start therapy quickly, without the stress:
Common Autism Sleeping Patterns in Children
No two autistic children sleep in exactly the same way. However, certain patterns show up consistently across research and clinical experience. If you recognize your child in this table, know that these patterns are understood and many of them are manageable.
Sleeping Pattern | What It Looks Like | Why It Happens |
Difficulty falling asleep | Takes 1–2+ hours to settle; frequent trips out of bed | Delayed melatonin, anxiety, overstimulation |
Night waking | Wakes 2–4+ times per night; hard to resettle | Light sleep cycles, sensory triggers, GI discomfort |
Early morning waking | Awake and active before 5 AM despite late bedtime | Disrupted circadian rhythm, low melatonin duration |
Unusual sleeping positions | Dinosaur hands, fetal curl, pressed against wall | Sensory input seeking, proprioceptive regulation |
Rocking or rhythmic movement | Self-rocks or head-rolls before or during sleep | Self-soothing stimming behavior |
Short total sleep time | Under 9 hours for school-age children | Combined effect of onset delay + night waking |
Did You Know? Autism Sleep Problems Can Start at Birth
Researchers in Italy found that one quarter of children with ASD in their study had experienced sleep and feeding problems since birth suggesting the causes are often biological rather than behavioral. [4]
What Is the "Dinosaur Hands" Sleeping Position in Autism?
You may have noticed your child sleeping with their wrists bent inward, elbows tucked close to their body, and fingers slightly curled toward their chest. This is often called the “dinosaur hands” or “T-rex arms” sleeping position and it is one of the most commonly discussed autism sleeping positions among parents and in the autism community online.
The position gets its name from the way it resembles the short, bent forearms of a T-Rex dinosaur. For many autistic children and adults, this is not something they consciously choose, it is how their body naturally positions itself when seeking comfort and security during sleep.
Read more: Understanding Hand Flapping in Autism: What Parents Should Know
Why Do Autistic Children Sleep with Bent Wrists?
There are several reasons this sleeping position is more common in autistic individuals than in neurotypical ones:
- Proprioceptive input: The body’s sense of its own position in space is often impaired in autism. Curling the arms inward gives the body a clear, grounded sense of where its limbs are which feels calming.
- Sensory regulation: Keeping arms close to the body reduces unexpected touch from bedding or surfaces, limiting unwanted sensory input during sleep.
- Stimming behavior: Tension and flexion of the body is a recognized form of stimming. The bent wrist position may provide rhythmic sensory feedback that helps the brain settle.
- Joint hypermobility: Many autistic individuals have looser joints. Curling the wrists inward may simply feel more comfortable and require less muscular effort.
- Is it harmful? Occasional T-rex arms sleeping is not medically harmful. However, if your child wakes with numbness, tingling, or wrist stiffness regularly, they may be compressing nerves in their wrists during the night. A body pillow or occupational therapist consultation can help address this without forcing an unnatural sleep position.
Other Common Sleeping Positions in Children with Autism
Beyond dinosaur hands, there are several other autism sleeping positions that parents frequently notice. Each one often serves a sensory or self-regulation purpose:
- Fetal position: Curled tightly into a ball with knees drawn to the chest provides deep pressure input and a sense of containment, often preferred by sensory-seeking children.
- Pressed against a wall or headboard: Sleeping flush against a hard surface provides consistent proprioceptive feedback throughout the night, which can be deeply calming.
- Face-down (prone sleeping): Pressure on the abdomen and face can provide intense sensory input. Note: monitor closely in very young children for safety.
- Starfish or spread-eagle: Some sensory-avoidant children prefer maximum space with no limbs touching the opposite of pressure-seeking.
- Constantly moving or repositioning: Frequent position changes through the night may reflect difficulty staying in comfortable deep sleep or mild restless leg symptoms.
Struggling to Figure Out Why Your Child Can't Sleep? A BCBA Can Help.
What Is Autism Sleep Regression and When Does It Happen?
You may have had a period where your child’s sleep improved then suddenly fell apart again. This is often called autism sleep regression. Unlike the sleep regressions typically seen in infants, sleep regression in autistic children can happen at any age and is often triggered by specific causes rather than developmental leaps alone.
Common triggers for autism sleep regression include:
- Changes in routine: new school year, move to a new home, change in therapy schedule
- Growth spurts or puberty: hormonal changes can significantly disrupt melatonin regulation
- Illness or medication changes: even temporary changes can shift sleep architecture
- Increased anxiety: social pressures, sensory overload from new environments or transitions
- Seasonal changes: shorter daylight hours in winter affect circadian cues
Sleep regression is rarely permanent. Returning to a consistent, structured sleep routine and eliminating new sensory disruptions often helps restore baseline sleep within two to four weeks.
Read More: Understanding Level 1 Autism: Early Signs, Challenges, and Support Strategies
Did You Know? Melatonin Can Increase Total Sleep Time by Over an Hour
A meta-analysis of 35 studies found that melatonin increased total sleep time by 73 minutes and reduced the time it takes to fall asleep by 66 minutes on average in children with ASD making it one of the most evidence-backed interventions available. [5]
How to Help Your Autistic Child Sleep Through the Night
There is no single fix but there is a highly effective combination of environmental, behavioral, and support strategies that work for most autistic children. [6] Start with the simplest adjustments before adding supplements or seeking medical intervention.
1. Build a Consistent Bedtime Routine
Predictability is one of the most powerful sleep tools for autistic children. A fixed sequence of activities such as bath, pajamas, dim lights, quiet activity, then bed signals to the brain that sleep is approaching. Aim for the routine to begin at the same time every night, including weekends. Visual schedules work especially well for children who struggle with verbal reminders.
2. Optimize the Sensory Environment
Audit your child’s bedroom for sensory triggers. Consider a white noise machine for children sensitive to sound, blackout curtains for light sensitivity, and weighted blankets for children who seek deep pressure input. The goal is to reduce unexpected sensory input and replace it with predictable, calming input the child can tolerate or even enjoy.
3. Limit Screens Before Bed
Blue light from screens suppresses melatonin production even in neurotypical people, the effect is stronger in children whose melatonin is already delayed. Set a firm screen-off rule at least 60 minutes before the start of the bedtime routine. Replace screen time with a low-stimulation activity your child enjoys.
Read More: How to Reduce Screen Time for Kids with Autism
4. Consider Melatonin (With Your Doctor’s Guidance)
Melatonin is the most research-supported supplement for autism sleep problems. Studies report that 86% of parents saw improvement in how quickly their child fell asleep after starting melatonin treatment. [7] Always discuss dosage, timing, and formulation with your child’s pediatrician before starting, as over-the-counter supplements vary significantly in purity and actual melatonin content.
5. Use ABA-Based Sleep Behavior Strategies
Applied Behavior Analysis is the first-line behavioral treatment recommended for sleep problems in children with ASD by the Sleep Committee of the Autism Treatment Network. [6] ABA strategies include structured bedtime routines, graduated extinction, positive reinforcement for staying in bed, and fading parental presence. A BCBA can create a personalized sleep plan for your child’s specific needs.
Best Sleep Aids for Autistic Children: What the Evidence Says
Sleep Aid | Evidence Level | How It Helps |
Consistent bedtime routine | Very Strong | Reduces anxiety, signals sleep onset |
Weighted blanket | Moderate | Deep pressure input, calming for sensory seekers |
White noise machine | Moderate | Blocks irregular sounds that trigger night waking |
Melatonin supplement (physician-guided) | Strong | Corrects delayed melatonin onset |
Blackout curtains | Moderate | Removes light cues that interfere with melatonin |
ABA sleep behavior plan | Very Strong | Addresses learned behaviors causing sleep resistance |
Occupational therapy | Moderate | Addresses sensory sensitivities disrupting sleep |
ABA Therapy Can Help Your Child Build Better Sleep Habits - Starting Now.
Is Rocking Yourself to Sleep a Sign of Autism?
Rocking before or during sleep, also called rhythmic movement disorder or body rocking, is more common in autistic children than in neurotypical peers, but it is not an autism-exclusive behavior. Many young children rock as a form of self-soothing. [8] In autistic children, it often persists beyond the toddler years and may be more intense.
Rocking before sleep is a form of stimming self-stimulatory behavior that helps regulate the nervous system. For autistic children, the rhythmic input is genuinely calming and helps the brain transition out of a hyper-alert state. On its own, it is not harmful and does not require intervention unless it disrupts sleep significantly or causes injury.
If rocking is combined with other signs of persistent social communication differences, repetitive behaviors across settings, sensory sensitivities it may be worth discussing an autism screening with your child’s pediatrician. One behavior alone is not a diagnosis.
Frequently Asked Questions
How do autistic people sleep differently from neurotypical people?
Autistic individuals are two to three times more likely to experience sleep problems than neurotypical people. [1] Common differences include taking longer to fall asleep (delayed sleep onset), waking more frequently during the night, sleeping fewer total hours, and adopting unusual sleeping positions. These differences are rooted in biology particularly melatonin dysregulation and sensory processing differences not behavior or routine alone.
What is the autistic baby sleeping position?
Autistic infants and toddlers may favor positions that provide proprioceptive input pressure and body awareness. Common ones include the fetal curl, pressing against a crib side, or sleeping with arms tucked close to the body. If you notice your baby consistently sleeping in unusual positions combined with other early signs of autism, speak with your pediatrician about a developmental screening.
Does sleeping with dinosaur hands mean my child has autism?
Not necessarily. The dinosaur hands or T-rex arms sleeping position can occur in neurotypical individuals too particularly those with sensory preferences, anxiety, or joint hypermobility. It is not a diagnostic criterion for autism. However, if it appears alongside persistent social communication differences, restricted interests, or repetitive behaviors, an evaluation would be appropriate.
What is the best sleep aid for autistic children?
The evidence most strongly supports a consistent, structured bedtime routine as the first step. [6] For children who still struggle, melatonin used under physician guidance has shown significant improvement in sleep onset and duration in multiple clinical trials. [5] Weighted blankets, white noise, and an ABA-based sleep behavior plan are valuable additional tools. Always consult your child’s doctor before starting any supplement.
Why does my autistic child keep waking up at night?
Night waking in autistic children often has multiple causes, lighter sleep architecture, sensory triggers (sounds, temperature, light), gastrointestinal discomfort, anxiety, or learned behaviors around seeking parental reassurance. A behavioral sleep assessment by a BCBA can identify which factors are driving the night waking for your specific child and create a structured plan to address them.
What is autism sleep regression?
Autism sleep regression refers to a period when a child who was previously sleeping reasonably well begins experiencing significant sleep problems again. It often follows changes in routine, puberty, illness, or new environmental stressors. Unlike infant sleep regressions, there is no fixed timeline. Returning to a structured routine and addressing any new anxiety sources usually helps restore sleep within a few weeks.
References
[1] Kennedy Krieger Institute, Interactive Autism Network. Sleep Problems in Children with Autism. kennedykrieger.org. Accessed 2025.
https://www.kennedykrieger.org/stories/interactive-autism-network-ian/sleep_problems
[2] Pagan C, Goubran-Botros H, Delorme R, et al. Disruption of melatonin synthesis is associated with impaired 14-3-3 and miR-451 levels in patients with autism spectrum disorder. Scientific Reports. 2017;7:2096.
https://pmc.ncbi.nlm.nih.gov/articles/PMC5437096/
[3] Yan M, Goldman RD. Melatonin for children with autism spectrum disorder. Canadian Family Physician. 2021;67(7):485–487. PMC8302336.
https://www.cfp.ca/content/66/3/183
[4] Malow BA, Katz T, Reynolds AM, et al. Sleep Difficulties and Their Relationship to Diagnosed Mental Health Conditions in Children with Autism Spectrum Disorders. Journal of Child Neurology. 2019.
https://pubmed.ncbi.nlm.nih.gov/31079275/
[5] Sung M, Chin CH, Loh JK, et al. (meta-analysis). In: An update on the cause and treatment of sleep disturbance in children and adolescents with autism spectrum disorder. Psychiatry Investigation. 2021. PMC8688794.
https://pmc.ncbi.nlm.nih.gov/articles/PMC8688794/
[6] Sleep Committee of the Autism Treatment Network. Behavioral Interventions as First-Line Treatment for Sleep Problems in ASD. Referenced in Yan M & Goldman RD (2021). PMC8302336.
https://pmc.ncbi.nlm.nih.gov/articles/PMC8302336/
[7] Cortesi F, Giannotti F, Ivanenko A, Johnson K. Sleep in children with autistic spectrum disorder. Sleep Medicine. 2010;11(7):659–664. doi:10.1016/j.sleep.2010.01.010. Child and Adolescent Psychiatry and Mental Health, BioMed Central, 2023.
https://ohsu.elsevierpure.com/en/publications/sleep-in-children-with-autistic-spectrum-disorder-2/
[8] Stores G, Wiggs L. Sleep Disturbance in Children and Adolescents with Disorders of Development. Clinics in Developmental Medicine. Mac Keith Press. Referenced by CDC autism clinical resources.
https://search.worldcat.org/title/sleep-disturbance-in-children-and-adolescents-with-disorders-of-development
[9] Martinez-Cayuelas E, et al. Melatonin Rhythm and Its Relation to Sleep and Circadian Parameters in Children and Adolescents with ASD. Frontiers in Neurology. 2022;13:813692. PMC9237227.
https://www.frontiersin.org/journals/neurology/articles/10.3389/fneur.2022.813692/full
[10] Malow BA, et al. Sleep and Autism: Current Research, Clinical Assessment, and Treatment Strategies. FOCUS: Journal of the American Psychiatric Association. 2024.
https://psychiatryonline.org/doi/full/10.1176/appi.focus.20230028

