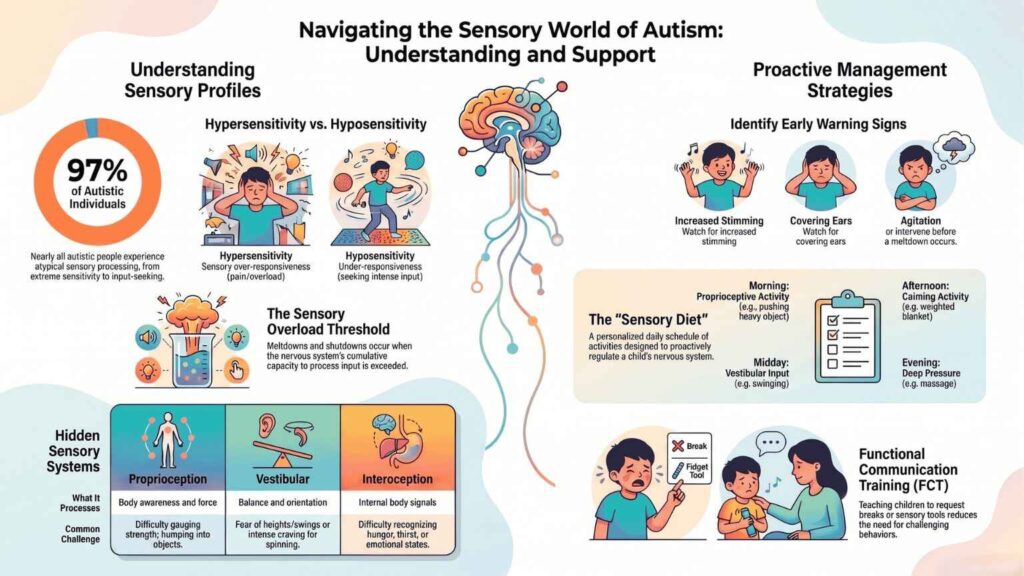
Sensory processing differences are one of the most common and most misunderstood aspects of autism spectrum disorder. Research shows that up to 97% of autistic individuals experience some form of atypical sensory processing, from extreme sensitivity to sound or touch, to actively seeking intense sensory input that others would find overwhelming. [1] These are not behavioral problems or attention-seeking. They reflect genuine differences in how the autistic brain receives and processes information from the environment. Understanding them is the first step to helping your child navigate the world with less distress and greater independence.
What Are Sensory Processing Differences in Autism?
The term sensory processing refers to how the brain receives, interprets, and responds to information coming in through the senses. For neurotypical individuals, this happens largely automatically and below conscious awareness. For many autistic people, this process is dysregulated either amplified to painful intensity or muted to the point where the input barely registers. [2]
Sensory processing differences have been part of the official diagnostic criteria for autism since the DSM-5 revision in 2013. [3] They fall into two main categories: hypersensitivity (over-responsiveness to sensory input) and hyposensitivity (under-responsiveness), and a single child can experience both simultaneously in different sensory systems.
Type | What It Means | Common Signs in Autistic Children |
Hypersensitivity (Over-responsive) | The brain amplifies sensory signals, input that feels mild to others feels intense, painful, or overwhelming | Covers ears at normal sounds, refuses certain textures or clothing tags, reacts strongly to specific smells, avoids crowds or bright lights, meltdowns in stimulating environments |
Hyposensitivity (Under-responsive) | The brain under-registers sensory signals, the child needs more input than usual to feel or notice stimulation | Seeks deep pressure (crashing, hugging tightly), mouths objects, unaware of pain or temperature, makes loud noises, spins or rocks to seek vestibular input |
Sensory Seeking | A specific form of hyposensitivity where the child actively seeks intense sensory experiences to regulate their nervous system | Constant movement, touching everything, strong preference for intense flavors or textures, repeatedly seeking certain sounds or visual patterns |
Read More: Helping Children with Sensory Processing Disorder
Your Child's Sensory Needs Can Be Addressed with Individualized ABA - Our BCBAs Are Ready.
Fill in the form below to discuss how your child could start therapy quickly, without the stress:
The 8 Sensory Systems - Not Just the Classic Five
Most people think of five senses. Autistic children can experience differences in eight sensory systems and the three beyond the classic five are especially important in autism and are among the most frequently misunderstood by parents and educators.
Sensory System | What It Processes | Common Challenge in Autism |
Auditory (Hearing) | Sounds, volume, frequency, background noise | Cannot filter background noise, fire alarms trigger panic, certain voices feel painful |
Visual (Sight) | Light, color, movement, depth | Fluorescent lights cause distress, difficulty with busy visual environments, overwhelmed by screens |
Tactile (Touch) | Pressure, texture, temperature, pain | Cannot tolerate clothing tags, specific fabric textures, unexpected touch from others |
Olfactory (Smell) | Odors, chemical compounds | Refuses rooms with certain smells, sensitive to perfumes, cleaning products, food odors |
Gustatory (Taste) | Flavor, texture, temperature of food | Extremely limited diet, texture aversions, gagging on certain foods |
Proprioception (Body Awareness) | Where the body is in space, force of movements | Difficulty gauging own strength, bumping into things, seeks crashing or deep pressure activities |
Vestibular (Balance & Movement) | Movement, balance, spatial orientation | Fear of swings or slides, or craves spinning and rocking that others find dizzying |
Interoception (Internal Body Sense) | Hunger, thirst, heart rate, temperature, pain from within | Cannot reliably recognize hunger, thirst, need to use the bathroom, or emotional states |
Interoception, the ability to sense what is happening inside the body, is increasingly recognized as a critical area for autistic individuals. [4] When a child cannot reliably feel hunger, thirst, or the early signs of emotional overwhelm, behavioral challenges that seem confusing from the outside often make complete sense once the interoceptive deficit is identified.
Did You Know?
When the DSM-5 was published in 2013, hyper- or hypo-reactivity to sensory input was formally added as one of the diagnostic criteria for autism spectrum disorder, not a side feature, but a core defining characteristic. A 2025 state-of-the-art review published in Brain Sciences confirmed sensory processing differences in up to 97% of autistic individuals, describing them as a ‘defining feature of the condition, shaping perception, cognition, and adaptive behavior.’ [1]
Sensory Overload, Meltdowns, and Shutdowns: What Is Actually Happening
A sensory meltdown is not a tantrum. It is not manipulation, defiance, or a failure of parenting. It is what happens when the autistic nervous system reaches its absolute limit of sensory input and loses the ability to self-regulate. [5] The child is not choosing to behave this way, the behavior is the direct result of a neurological system that has been overwhelmed beyond its capacity to cope.
Two types of reactions occur when the threshold is crossed. A meltdown is an externalized response, crying, screaming, dropping to the floor, hitting, or throwing objects. A shutdown is an internalized response, the child goes quiet, withdraws, stops communicating, and may appear to ‘shut down’ completely. Both are equally valid signs of sensory overload and both require the same first response: reduce the sensory input immediately.
Early Warning Signs of Sensory Overload Before the Threshold Is Crossed
- Covering ears: even briefly, in response to sounds that seem normal to others
- Increased stimming: flapping, rocking, spinning, repeating words or sounds, these are self-regulation tools, not symptoms to suppress
- Requesting to leave: in any form, verbal or nonverbal, this is communication that must be honored
- Visible discomfort: pulling at clothes, refusing to enter a room, crying without apparent trigger
- Increasing agitation: shorter responses, refusal to engage, irritability rising rapidly
- Seeking deep pressure: crawling under furniture, hugging tightly, pressing into walls or corners
Recognizing these signs and responding before the threshold is crossed prevents meltdowns. The window between the first signs and full overload is your intervention opportunity.
How ABA Therapy Addresses Sensory Challenges
Applied Behavior Analysis addresses autism sensory issues by first identifying the function of each sensory-related behavior through a Functional Behavior Assessment (FBA). [6] Not every sensory behavior serves the same purpose, some are escape behaviors, some are self-reinforcing, and some are communication of genuine distress. Treatment must be matched to the function, not applied generically.
The core ABA strategies used for sensory challenges include:
Systematic Desensitization
For children with hypersensitivity, gradual exposure to the triggering stimulus at very low intensity with consistent positive reinforcement for tolerating each step builds sensory tolerance over time. [7] This is not forcing a child to endure something that hurts them. It is a carefully paced, data-driven process where the child controls the pace through their observable responses.
Read More: Understanding Stimulus Control in Autism Therapy
Sensory Diet Programming
A sensory diet is not about food, it is a personalized schedule of sensory activities built into the child’s day to regulate their nervous system proactively. [7] Designed collaboratively between a BCBA and occupational therapist, a sensory diet might include scheduled movement breaks, deep pressure activities, proprioceptive input exercises, or specific calming routines before high-stimulation transitions.
Read More: ABA vs OT: What’s the Difference and Does Your Child Need Both?
Functional Communication Training (FCT) for Sensory Needs
Many sensory-related behaviors, covering ears, meltdowns, and refusal are a child’s only available communication tool for expressing ‘this is too much.’ [6] FCT directly addresses this by teaching the child an appropriate replacement behavior: requesting a break, handing a break card, or indicating that a sensory tool is needed. When a child can communicate their sensory needs, the intensity and frequency of challenging behaviors consistently decrease.
Read More: Functional Communication Training in ABA
Environmental Modification and Parent Training
At ABS, parent training is a central component of all sensory programming. When families understand their child’s sensory profile, which inputs are triggers, which are regulating, and what the early warning signs look like, they can modify the environment proactively and intervene early rather than reactively. [6] This means adjustments like creating a designated sensory break space, using noise-canceling headphones in certain environments, adjusting lighting, or pre-preparing the child for transitions with visual schedules.
Did You Know?
A 2025 state-of-the-art review in Brain Sciences found that sensory processing differences in autism do not exist in isolation, they directly interact with co-occurring conditions including anxiety, ADHD, and sleep and feeding difficulties. A child whose sleep is disrupted by sensory sensitivities will have a significantly lower sensory threshold the following day. Addressing sensory regulation often produces improvements in multiple co-occurring challenges simultaneously. [1]
Practical Sensory Strategies for Families - Starting This Week
These are evidence-informed starting points. Always work with your child’s BCBA or occupational therapist to tailor these to your child’s specific sensory profile:
Challenge | Practical Strategy | Why It Helps |
Auditory hypersensitivity (sounds) | Noise-canceling headphones for high-stimulation environments; advance warning before loud events; identifying low-stimulation routes in stores or buildings | Reduces the amplitude of triggering input; gives the child control over their own experience |
Tactile hypersensitivity (touch, clothing) | Seamless socks, tagless clothing; let child choose own fabric textures; practice of slow, predictable touch rather than unexpected contact | Removes chronic irritants from the sensory baseline; reduces ‘sensory load’ the child carries all day |
Proprioceptive seeking (crashing, jumping) | Scheduled heavy work: wall push-ups, carrying books, jumping on a trampoline; a sensory diet that provides this input proactively | Meets the nervous system’s need for input in a safe, structured way, reducing disruptive seeking behaviors |
Vestibular seeking (spinning, rocking) | Scheduled swing time, rocking chair, rolling on a therapy ball before demanding tasks | Provides regulatory input before high-demand activities, improving attention and self-regulation |
Sensory meltdowns in public | Identify early warning signs; designate an exit plan before arrival; noise-canceling headphones in bag; ‘first-then’ visual schedule for the outing | Prevention is always more effective than intervention after the threshold is crossed |
Food texture aversions | Systematic food exposure with no pressure; food chaining (starting from accepted foods and gradually expanding texture/flavor); positive reinforcement for exploration | Builds tolerance without trauma, forced exposure to rejected foods reliably worsens aversions |
How ABS Can Help Your Child Navigate Sensory Challenges
At Achievement Behavior Services, every ABA program begins with a comprehensive assessment that includes the child’s sensory profile. Our BCBAs work collaboratively with families and, where appropriate, with occupational therapists, to develop sensory-informed ABA programs that address the root cause of behavior, not just its surface appearance. We serve families across New York, New Jersey, Connecticut, Georgia, and North Carolina, with in-home services and center-based locations in Malverne, NY and Douglasville, GA.
Ready to Build a Sensory-Informed ABA Program for Your Child? ABS BCBAs Are Here to Help.
Frequently Asked Questions
Q: What percentage of autistic people have sensory issues?
Research estimates that 90–97% of autistic individuals experience some form of atypical sensory processing. [1] A 2025 state-of-the-art review in Brain Sciences described sensory processing differences as a ‘defining feature’ of autism, noting that they shape perception, cognition, and adaptive behavior. Sensory differences have been part of the official DSM-5 autism diagnostic criteria since 2013. [3]
Q: What is the difference between hypersensitivity and hyposensitivity in autism?
Hypersensitivity means the brain over-registers sensory signals, input that feels normal to others feels painful, overwhelming, or intolerable to the autistic person. [2] Examples include covering ears at normal sounds, refusing certain fabric textures, or reacting strongly to specific smells. Hyposensitivity means the brain under-registers input, the child needs more stimulation than usual to feel it, often leading to sensory seeking behaviors like crashing, spinning, or mouthing objects. A single child can be hypersensitive in some systems and hyposensitive in others simultaneously.
Q: What causes sensory overload in autism?
Sensory overload occurs when the cumulative amount of sensory input across all systems exceeds the autistic nervous system’s capacity to process and regulate it. [5] Every day’s sensory experiences build on each other, a child who has already been managing loud environments, uncomfortable clothing, and fluorescent lights for hours will have a much lower threshold than a well-rested child in a calm environment. It is the total sensory load across the day, not just a single trigger, that typically produces a meltdown or shutdown.
Q: How does ABA therapy help with autism sensory issues?
ABA therapy addresses sensory issues by first conducting a Functional Behavior Assessment to identify the specific function of each sensory-related behavior. [6] From there, BCBAs use strategies including systematic desensitization (gradual, reinforced exposure to triggering stimuli), sensory diet programming (proactive sensory regulation throughout the day), Functional Communication Training (teaching appropriate ways to request breaks or communicate sensory needs), and environmental modifications. Parent training is central, when families understand their child’s sensory profile and early warning signs, they can prevent most meltdowns before they escalate.
Q: What is a sensory diet for autism?
A sensory diet is a personalized, scheduled program of sensory activities built into a child’s daily routine to proactively regulate their nervous system. [7] It is not related to food, the term ‘diet’ refers to the tailored ‘dosage’ of sensory input the child receives. A sensory diet is designed collaboratively between a BCBA and occupational therapist, and may include heavy work activities (pushing, pulling, carrying), scheduled movement breaks, deep pressure input, or specific calming routines before transitions. When implemented consistently, a sensory diet reduces the frequency and intensity of sensory-driven challenging behaviors.
Q: Can sensory issues in autism improve over time?
Yes, with targeted intervention, most autistic children can build sensory tolerance and develop effective self-regulation strategies. [6] The goal is not to eliminate sensory differences, which are a genuine neurological feature of autism, but to reduce the degree to which they interfere with daily life and participation. With consistent ABA support, parent training, and where appropriate OT collaboration, many children make significant gains in their ability to tolerate previously overwhelming environments and communicate their sensory needs before reaching the overload threshold.
References
[1] Narzisi A, et al. Sensory processing in autism: a call for research and action. Frontiers in Psychiatry. 2025;16:1584893.
https://www.frontiersin.org/journals/psychiatry/articles/10.3389/fpsyt.2025.1584893/full
[2] Marco EJ, Hinkley LBN, Hill SS, Nagarajan SS. Sensory processing in autism: a review of neurophysiologic findings. Pediatric Research. 2011;69(5 Pt 2):48R–54R. https://pmc.ncbi.nlm.nih.gov/articles/PMC3086654/
[3] American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5). APA, 2013. Sensory criteria added as criterion B4.
https://www.psychiatry.org/psychiatrists/practice/dsm
[4] Mahler KJ. Interoception: The Eighth Sensory System. AAPC Publishing, 2015. Referenced in: Frontiers in Psychiatry sensory review, 2025.
https://www.frontiersin.org/journals/pediatrics/articles/10.3389/fped.2025.1720179/full
[5] Randell E, Wright M, Milosevic S, et al. Sensory integration therapy for children with autism and sensory processing difficulties: the SenITA RCT. Health Technology Assessment. 2022;26(29). NCBI Bookshelf:
https://www.ncbi.nlm.nih.gov/books/NBK581602/
[6] Cooper JO, Heron TE, Heward WL. Applied Behavior Analysis (3rd ed.). Pearson, 2020. Referenced through: Association for Behavior Analysis International (ABAI).
https://www.abainternational.org/welcome.aspx
[7] Schaaf RC, Mailloux Z. Clinician’s Guide for Implementing Ayres Sensory Integration: Promoting Participation for Children With Autism. AOTA Press, 2015.
https://library.aota.org/Clinicians_Guide_for_Implementing_Ayres_SI/
[8] Cascio CJ, et al. Tactile perception in adults with autism: a multidimensional psychophysical study. Journal of Autism and Developmental Disorders.
https://pubmed.ncbi.nlm.nih.gov/17415630/
[9] Shaw KA, et al. Prevalence and Early Identification of ASD — ADDM Network, 2022. MMWR Surveillance Summaries. 2025;74(SS-2). CDC. https://www.cdc.gov/mmwr/volumes/74/ss/pdfs/ss7402a1-H.pdf
[10] Cottini M, et al. Sensory Phenotypes in Autism Spectrum Disorder Associated with Distinct Patterns of Social Communication, Repetitive and Restrictive Behaviors or Interests, and Comorbidities: A State-of-the-Art Review. Brain Sciences. 2025;16(1):53.
https://www.mdpi.com/2076-3425/16/1/53

