Applied Behavior Analysis (ABA) is a scientifically validated therapy rooted in the principles of learning and behavior. It is recognized by the U.S. Surgeon General and the American Psychological Association as an evidence-based best practice for autism spectrum disorder. [1] ABA works by applying what research tells us about how behavior is learned and changed, using positive reinforcement to increase helpful skills and reduce behaviors that interfere with daily life. More than 20 controlled studies have established that intensive, long-term ABA therapy improves outcomes in language development, intellectual functioning, daily living skills, and social communication for children with autism. [2]
Whether you are a parent hearing about ABA for the first time, or someone who wants to understand the science behind it, this guide breaks down everything: what ABA is, how it works, the techniques involved, who delivers it, and what the research actually says.
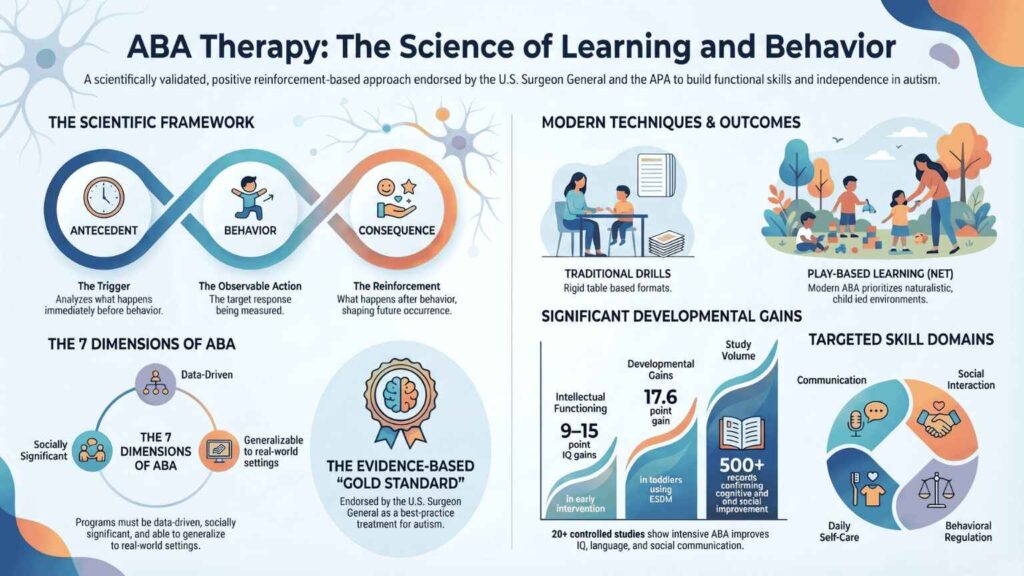
The Scientific Definition: What Is Applied Behavior Analysis?
Applied Behavior Analysis is the practical application of the science of behaviorism, the study of how the environment influences behavior to real-world problems. It was formally defined and established as a discipline in 1968 by Baer, Wolf, and Risley in their landmark paper in the Journal of Applied Behavior Analysis. [3] Their framework established that ABA must be both applied (focused on socially significant behaviors) and analytic (driven by data and measurable outcomes).
ABA therapists have worked with children with autism since the 1960s, when Dr. O. Ivar Lovaas first applied behavioral principles to teach communication and reduce harmful behaviors in children with developmental disabilities. [4] Since then, the field has evolved dramatically moving away from rigid, table-based drill formats toward naturalistic, play-based, and child-directed approaches that prioritize the child’s comfort, interests, and quality of life.
Read More: The Growing Impact of Applied Behavior Analysis (ABA) Therapy
Have Questions About Starting ABA for Your Child? Our BCBAs Are Ready to Help.
Fill in the form below to discuss how your child could start therapy quickly, without the stress:
The 7 Dimensions of ABA: The Scientific Framework
Baer, Wolf, and Risley’s 1968 definition established 7 core dimensions that every ABA intervention must meet to be considered genuine applied behavior analysis. These dimensions are what separate evidence-based ABA from general behavioral approaches. [3]
|
Dimension |
What It Means |
Why It Matters |
|
1. Applied |
Focuses on behaviors that are socially significant and meaningful to the individual’s real life |
Therapy addresses skills that genuinely improve the person’s daily functioning and independence |
|
2. Behavioral |
Targets specific, observable, and measurable behaviors — not vague traits or internal states |
Goals can be tracked with data, and progress can be objectively verified |
|
3. Analytic |
Every intervention is based on systematic data collection demonstrating a reliable relationship between the treatment and behavior change |
Decisions are driven by evidence, not guesswork — if the data doesn’t show progress, the approach changes |
|
4. Technological |
Procedures are described precisely enough that any trained practitioner could replicate them |
Ensures consistency across therapists, settings, and time — critical for families working with multiple providers |
|
5. Conceptually Systematic |
Techniques are derived from and explained by established principles of behavior science |
Connects practice to a scientific foundation — interventions can’t be ad hoc or invented without theoretical grounding |
|
6. Effective |
The intervention must produce meaningful, practical change in the client’s life |
A statistically significant result that doesn’t change real-world functioning is not sufficient |
|
7. Generality |
Skills learned in therapy must generalize to other settings, people, and situations not present during training |
A child who can request food only with their ABA therapist but not with a teacher has not truly acquired the skill |
Read Full Guide: The 7 Dimensions of ABA Therapy Explained: A Complete Parent’s Guide
How Does ABA Therapy Work? The ABC Foundation
Every ABA program is built on the ABC model Antecedent, Behavior, Consequence. This three-part framework is how behavior analysts understand why behaviors occur and how to change them. [5]
- Antecedent (A): What happens immediately before a behavior, the trigger, prompt, or setting event. Example: a parent asks a child to put their shoes on.
- Behavior (B): The specific, observable, and measurable action that occurs. Example: the child ignores the request and continues playing.
- Consequence (C): What happens immediately after the behavior, which determines whether it will happen again. Example: the parent repeats the request (attention consequence that reinforces ignoring).
By analyzing the A-B-C chain, a BCBA identifies the function of the behavior and the reason it keeps happening. The four most common functions are: attention, escape from demands, access to something desired, and automatic sensory reinforcement. Once the function is understood, the BCBA designs an intervention that teaches a replacement behavior serving the same function but in a more appropriate way. This is called Functional Communication Training (FCT).
What Does ABA Therapy Aim to Do?

The goal of ABA therapy is not to change who a child is or to suppress behaviors that are simply different. Modern ABA focuses on building skills that increase independence, safety, and quality of life and reducing behaviors that cause harm to the child or others. [1]
ABA programs target skill development across these core domains:
|
Skill Domain |
What ABA Teaches |
Example Goal |
|
Communication & Language |
Expressive language, requesting, labeling, conversation, AAC use |
Child will use 3-word phrases to request preferred items in 4 out of 5 opportunities |
|
Turn-taking, joint attention, peer interaction, reading social cues, emotional recognition |
Child will initiate play with a peer using a verbal greeting in 3 of 5 playground opportunities |
|
|
Daily Living & Self-Care |
Dressing, grooming, meal preparation, toilet training, household routines |
Child will independently complete a 5-step handwashing routine with no prompting |
|
Academic & Pre-Academic |
Following instructions, attending to tasks, reading readiness, number concepts |
Child will identify 10 sight words with 90% accuracy across 3 consecutive sessions |
|
Behavior Regulation |
Identifying emotions, coping with frustration, tolerating transitions, reducing meltdowns |
Child will use a visual break card instead of aggression when frustrated in 4 of 5 observations |
|
Adaptive & Independence Skills |
Community safety, transportation, money skills, job readiness for older learners |
Teen will independently navigate a familiar public transit route with verbal recall of 3 safety rules |
Did You Know?
Applied Behavior Analysis is designated an ‘evidence-based best practice treatment’ by the U.S. Surgeon General and the American Psychological Association making it the most rigorously validated behavioral intervention for autism spectrum disorder in existence. More than 20 controlled studies have established its effectiveness across language, cognitive, social, and daily living outcomes. [1]
Core ABA Techniques: What Happens in a Session
Modern ABA draws from a range of evidence-based techniques. The approach selected for any individual child depends on their age, learning profile, and specific goals. Here are the most widely used:
Discrete Trial Training (DTT)
DTT is a structured, one-on-one teaching format that breaks complex skills into small, discrete components. Each component is presented as a clear instruction, the child responds, and correct responses are immediately reinforced. [4] DTT is most effective for building foundational skills like imitation, receptive language, and matching, particularly with young children in the early stages of intervention. It is delivered in a massed-trial format with clear antecedents and consistent reinforcement.
Natural Environment Teaching (NET)
NET embeds learning opportunities into the child’s natural play and daily routines, following the child’s motivation and interest. Instead of a structured desk session, the BCBA or RBT creates teaching moments during activities the child is already engaged in. [5] NET is particularly effective for communication generalization because skills are learned in the same context they will be used, transfer to real life happens faster. It is the preferred format for toddlers and young children with early ASD.
Pivotal Response Treatment (PRT)
PRT targets ‘pivotal’ areas of development motivation, self-initiation, self-management, and response to multiple cues where gains produce cascading improvements across many other skill areas simultaneously. [4] PRT is naturalistic and child-led: it uses the child’s interests to create high-motivation learning opportunities, reducing the compliance pressure of traditional structured programs.
Early Start Denver Model (ESDM)
ESDM integrates ABA principles with developmental and relationship-based approaches and is specifically designed for children aged 12–48 months. [6] It is delivered during play and daily routines, with each activity targeting multiple developmental goals simultaneously. Randomized controlled trials published in peer-reviewed journals have demonstrated ESDM’s effectiveness in improving IQ, language, and adaptive behavior in toddlers.
Functional Communication Training (FCT)
FCT is one of the most evidence-based strategies for reducing challenging behaviors. It works by identifying the function a behavior serves such as escaping a demand or gaining attention and then teaching the child a communicative replacement behavior that achieves the same outcome more appropriately. [5] Example: a child who bites to escape a task is taught to hand over a ‘break card’ instead. Both behaviors serve the same function; only one is safe and acceptable.
Who Provides ABA Therapy? The Clinical Team
ABA therapy is delivered by a tiered clinical team, each with specific training, credentials, and responsibilities. Understanding this structure helps families know exactly who is working with their child and why.
|
Team Member |
Credential |
Role in ABA Therapy |
|
BCBA (master’s degree + exam + supervised fieldwork) |
Designs the treatment program, conducts FBAs, writes behavior intervention plans, supervises the team, trains parents the clinical decision-maker |
|
|
Doctoral Behavior Analyst |
BCBA-D (doctoral degree) |
Same as BCBA but may also lead research, training, and consultation often found in clinical director or leadership roles |
|
Board Certified Assistant Behavior Analyst |
BCaBA (bachelor’s degree) |
Assists in program design and implementation under BCBA supervision; can supervise RBTs |
|
RBT (40-hour training + exam) |
Delivers direct therapy to the child under BCBA supervision, the person the child sees most frequently in sessions |
At Achievement Behavior Services (ABS), every ABA program is designed and supervised by a BCBA. Our RBTs work under direct BCBA oversight, and all programs are reviewed regularly with data-driven adjustments. Parents receive regular coaching so that skills learned in therapy carry over into the home throughout the day.
ABS BCBAs Design Every Program, No Cookie-Cutter Templates, Only Individualized ABA.
What Does the Research Say? The Evidence Behind ABA
ABA is among the most extensively studied behavioral interventions in all of psychology. Here is what decades of controlled research has established:
|
Research Finding |
Source / Study |
|
More than 20 controlled studies confirm that intensive ABA (25–40 hours/week for 1–3 years) produces meaningful gains in IQ, language, adaptive behavior, and social skills for children with autism |
U.S. Surgeon General Report, endorsed by APA |
|
ESDM randomized controlled trial: children (18–30 months) showed 17.6-point developmental gain vs 7.0 in the comparison group after 2 years of intervention |
Dawson et al., Pediatrics 2010, PMC6034700 |
|
ABA scoping review of 551 study records: 66–68% of studies on children aged 0–5 years reported improvement in cognitive, language, and social/communication outcomes |
Linstead et al., PMC9458805, 2022 |
|
Narrative review (2025): EIBI initiated between 18 and 36 months produces IQ gains of 9–15 points and significantly stronger language and adaptive behavior outcomes |
PMC12514992, 2025 |
|
JAMA Pediatrics meta-analysis (2024) of 9,038 children: more intervention hours at younger ages are associated with significantly better developmental outcomes across all domains |
Sandbank et al., JAMA Pediatrics 2024, pubmed/38913359 |
|
ABA therapy effectiveness for expressive language: large effect size confirmed across 14 RCTs in meta-analysis |
PMC7265021, ABA Meta-Analysis Review |
Did You Know?
The research that earned ABA the U.S. Surgeon General’s endorsement specifically established that ‘intensive and long-term therapy defined as 25 to 40 hours per week for 1 to 3 years shows gains in intellectual functioning, language development, daily living skills, and social functioning. Intensity and consistency are the two variables most directly linked to positive outcomes across all published studies. [2]
Is ABA Only for Autism? Who Else Can It Help?
While ABA is most commonly associated with autism, the science of behavior it applies to is universal. ABA has been successfully used for children and adults with:
- Autism Spectrum Disorder (ASD): the most common and researched application, supported by the strongest evidence base
- Intellectual and developmental disabilities: teaching daily living, communication, and adaptive skills
- ADHD: building attention, task completion, and behavioral self-regulation through structured reinforcement
- Language and speech delays: especially for children who are minimally verbal or nonverbal
- Traumatic brain injury: relearning functional behaviors and communication following neurological injury
- Organizational Behavior Management (OBM): ABA principles applied in corporate and healthcare settings to improve workplace safety and performance
Does Insurance Cover ABA Therapy?
Yes, in most cases. All 50 U.S. states now require Medicaid plans to cover ABA therapy for children with autism who have a medical necessity determination. [7] Many private insurance plans are also required to provide ABA coverage under state mandates. All Medicaid plans must cover ABA for children under 21 when a physician has determined it is medically necessary.
Coverage details vary by plan, state, and provider. At ABS, our team works directly with families to verify insurance benefits and navigate the authorization process so that access to care is not delayed by administrative barriers.
What Are the Criticisms of ABA and How Has the Field Responded?
ABA has attracted both strong support and meaningful criticism within the autism community. As a field, we believe both deserve honest engagement because understanding the history and evolution of ABA helps families make genuinely informed decisions about care.
Early forms of ABA, developed in the 1960s, used punishment alongside reinforcement including practices that are considered harmful and unethical today. [4] Some autistic self-advocates have raised concerns that certain ABA programs focused more on making autistic children appear neurotypical than on improving their genuine quality of life.
Here is how modern, evidence-based ABA has directly responded to each major criticism:
|
Criticism |
How Modern ABA Responds |
|
Early ABA used punishment and aversive procedures |
Punishment is no longer used in any reputable ABA program. The BACB’s Ethics Code (revised 2022) explicitly prohibits harmful procedures. Modern ABA is built on positive reinforcement only |
|
ABA tries to eliminate behaviors that are natural for autistic people (stims, special interests) |
Contemporary ABA explicitly distinguishes between behaviors that cause harm and behaviors that are simply different. Harmless stims and special interests are not suppressed — they are often used as reinforcers |
|
ABA is too focused on compliance |
Modern approaches (NET, PRT, ESDM) are child-led, play-based, and motivation-driven. The child’s preferences guide the session, not a rigid protocol |
|
ABA ignores the autistic person’s perspective |
Best-practice ABA now integrates autistic voices in goal-setting and consent, particularly for older learners. Self-advocacy goals are increasingly included in programs |
At Achievement Behavior Services, we practice strengths-based, compassionate ABA, which means every program begins with what the child can do, uses their interests as the foundation of motivation, and is always evaluated by whether it is genuinely improving the child’s life. Therapy should never make a child afraid of coming to sessions. If it does, something is wrong.
What Should Families Expect from the ABA Process?
The ABA journey from referral to active therapy typically follows these steps:
- Referral and insurance verification. Your pediatrician, developmental specialist, or school team may refer your child. Your insurance benefits are verified to understand coverage and authorization requirements.
- BCBA intake and assessment. A qualified BCBA meets with your family to understand your child’s strengths, challenges, and your family’s goals. They observe your child and gather input from caregivers and teachers.
- Functional Behavior Assessment (FBA). For children with behavioral challenges, the BCBA conducts a systematic assessment to identify the cause and function of specific behaviors before designing any intervention.
- Treatment plan development. The BCBA writes an individualized program: skill acquisition goals, behavior intervention plans (if needed), parent training components, and recommended therapy hours.
- Active therapy and data collection. RBTs work directly with your child while collecting session-by-session data. The BCBA reviews data regularly and adjusts the program based on what is working.
- Parent training and generalization. You learn the same techniques being used in sessions so that skills are practiced throughout the day not just during therapy hours. Generalization is built in from the start.
- Progress reviews and program updates. The BCBA meets with you regularly to review progress, celebrate milestones, and plan next goals. Programs evolve as your child grows.
ABS Serves Families Across NY, NJ, CT, GA & NC - Start the ABA Conversation Today.
ABS Provides In-Home Early Intervention ABA Across NY, NJ, CT, GA & NC – Centers in Malverne, NY and Douglasville, GA.
- New York – In-home and center-based ABA therapy
- New Jersey – ASD evaluations and individualized ABA programs
- Connecticut – Evidence-based autism support for families
- Georgia – Personalized ABA therapy for lasting results
- North Carolina – Supporting your child’s development journey
- Douglasville, GA – Family-centered autism care
How to Choose a Quality ABA Provider: What to Look For
Not all ABA programs are equal. These are the signs of a high-quality, ethical provider:
- Every program is supervised by a credentialed BCBA: not just managed by administrative staff
- Written, individualized treatment plan: not a generic template applied to every child
- Regular BCBA supervision of RBTs: BACB guidelines require a minimum of 5% of total therapy hours in direct observation
- Data collected every session: and shared with parents in a format they can understand
- Parent training built into the program: not an optional add-on
- Positive, naturalistic sessions: your child should not dread going to therapy. Play, motivation, and comfort matter
- Transparent about the controversy: a quality provider welcomes honest questions about ABA’s history and addresses them directly
Red Flags to Watch for in Any ABA Program
- High RBT caseloads with minimal BCBA contact, find out how often the BCBA directly observes your child
- Programs that cannot clearly explain the function of your child’s challenging behaviors
- No parent training component, you are your child’s most important teacher
- Sessions your child actively resists attending or that cause visible distress
- Programs that focus entirely on compliance and following instructions without skill-building
- No data sharing, you should be able to see your child’s progress data at any time
Frequently Asked Questions
Q: What is the definition of Applied Behavior Analysis?
Applied Behavior Analysis (ABA) is the scientific application of behavioral principles rooted in the study of how the environment influences behavior to socially significant problems. It uses systematic data collection, positive reinforcement, and evidence-based techniques to increase helpful behaviors and skills, and reduce behaviors that interfere with learning or safety. [1] It is the most extensively researched behavioral intervention for autism spectrum disorder, endorsed by the U.S. Surgeon General and the American Psychological Association.
Q: How does ABA therapy work for autism?
ABA therapy for autism works by applying the ABC model (Antecedent-Behavior-Consequence) to understand why behaviors occur, then designing individualized programs that teach replacement skills and reinforce positive behaviors. A BCBA assesses the child, identifies the functions of challenging behaviors, sets measurable goals, and supervises an RBT team that works directly with the child. Data is collected every session and the program adjusts continuously based on what the data shows.
Q: What are the 7 dimensions of Applied Behavior Analysis?
The 7 dimensions Applied, Behavioral, Analytic, Technological, Conceptually Systematic, Effective, and Generality, were established by Baer, Wolf, and Risley in 1968 and define what separates genuine ABA from general behavioral approaches. [3] An intervention must meet all 7 criteria: it must target meaningful behaviors, be measurable, be evidence-driven, be replicable, be grounded in behavioral science, produce real-world change, and produce skills that transfer to new settings and people.
Q: How many hours of ABA therapy does a child with autism need?
The research that earned ABA the U.S. Surgeon General’s endorsement defined ‘intensive’ ABA as 25 to 40 hours per week for 1 to 3 years. [2] However, the right intensity depends on the child’s age, severity of delays, and specific goals. A 2024 JAMA Pediatrics meta-analysis of 9,038 children confirmed that more hours at younger ages are associated with significantly better outcomes. Your BCBA will recommend the appropriate level after a comprehensive assessment.
Q: Is ABA therapy harmful?
Early forms of ABA from the 1960s used punishment procedures that are now considered unethical and are not used in any reputable ABA program. [4] Modern ABA as practiced under the BACB’s updated Ethics Code (2022) is built entirely on positive reinforcement, respects autistic identity, and is increasingly child-led and play-based. When delivered by a qualified BCBA who prioritizes the child’s wellbeing, ABA should not cause distress. If it does, that is a red flag about the specific provider, not about ABA as a science.
Q: How is ABA different from other autism therapies?
ABA is distinct from speech therapy, occupational therapy, and developmental therapies in that it is explicitly driven by data, requires systematic behavioral assessment before any intervention, and derives all techniques from established principles of behavioral science. [5] ABA can also incorporate goals from other disciplines: communication, fine motor, social skills but delivers them through a behavioral learning framework. At ABS, our BCBAs collaborate with speech therapists, school teams, and other providers to ensure all therapy goals are aligned.
References
[1] Autism Speaks. Applied Behavior Analysis (ABA). U.S. Surgeon General and APA designation. https://www.autismspeaks.org/applied-behavior-analysis
[2] U.S. Surgeon General. Mental Health: A Report of the Surgeon General. ABA evidence base — 20+ controlled studies. Washington, DC: U.S. Dept of Health and Human Services, 1999. Endorsed ongoing by APA.
https://profiles.nlm.nih.gov/spotlight/nn/catalog/nlm:nlmuid-101584932X120-doc
[3] Baer DM, Wolf MM, Risley TR. Some current dimensions of applied behavior analysis. Journal of Applied Behavior Analysis. 1968;1(1):91–97.
https://onlinelibrary.wiley.com/doi/10.1901/jaba.1968.1-91
[4] Child Mind Institute. What Is Applied Behavior Analysis (ABA)? Updated August 2025.
https://childmind.org/article/what-is-applied-behavior-analysis/
[5] Cooper JO, Heron TE, Heward WL. Applied Behavior Analysis (3rd ed.). Pearson, 2020. Referenced in: Association for Behavior Analysis International (ABAI).
https://www.pearson.com/en-us/subject-catalog/p/applied-behavior-analysis/P200000000905/9780137477210
[6] Dawson G, et al. Randomized, Controlled Trial of an Intervention for Toddlers With Autism: The Early Start Denver Model. Pediatrics. 2010;125(1). PMC6034700. https://pmc.ncbi.nlm.nih.gov/articles/PMC6034700/
[7] Autism Speaks. Insurance Resources — State Mandates and Medicaid Coverage for ABA Therapy. https://www.autismspeaks.org/health-insurance
[8] Linstead E, et al. Applied Behavior Analysis in Children and Youth with ASD: A Scoping Review. PMC9458805. 2022.
https://pmc.ncbi.nlm.nih.gov/articles/PMC9458805/
[9] Sandbank M, et al. Determining Associations Between Intervention Amount and Outcomes for Young Autistic Children: A Meta-Analysis. JAMA Pediatrics. 2024;178(8):763–773. https://pubmed.ncbi.nlm.nih.gov/38913359/
[10] Behavior Analyst Certification Board (BACB). Ethics Code for Behavior Analysts. Revised 2022. https://www.bacb.com/ethics-information/ethics-codes/

