Most parenting advice for autism families sounds the same: be patient, be consistent, celebrate small wins. That advice is not wrong but it is incomplete. The parents who make the most measurable difference in their autistic child’s progress are the ones who learn to use the same ABA-based strategies their child’s therapists use not just during scheduled sessions, but throughout the entire day. Research shows that parent-implemented ABA interventions significantly improve outcomes in communication, behavior, and daily living skills when caregivers are properly trained.[1]
This guide covers 6 specific strategies that BCBAs teach in parent training, written in plain language so you can start using them at home this week.
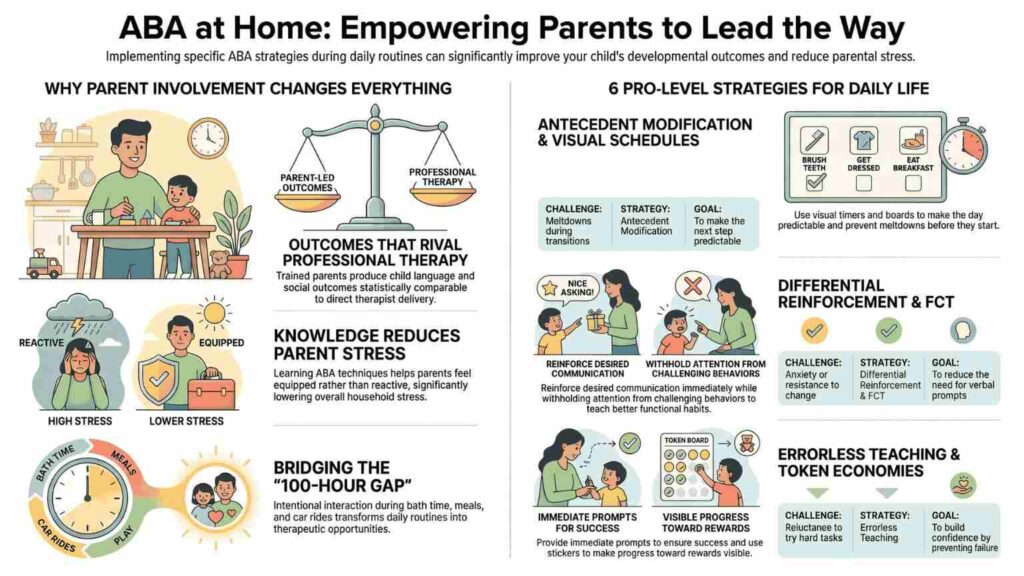
Why Parent Involvement Is One of the Strongest Predictors of Progress?
An autistic child who receives 20 hours of ABA therapy per week still has approximately 100 waking hours that week without a therapist. What happens in those hours matters enormously. A landmark meta-analysis published in Pediatrics found that parent-mediated interventions produced significant improvements in child language and social communication outcomes comparable in some domains to direct therapist-delivered intervention.[2]
Did You Know?
A 2023 meta-analysis of parent-mediated ABA interventions found that parents who received structured coaching from a BCBA produced child outcomes in language and social communication that were statistically comparable to those from direct therapist delivery and that combined models (therapist + trained parent) produced the strongest results of all.[2]
This is why parent training is not an optional add-on at evidence-based ABA providers, it is a clinical requirement. The BACB’s guidelines identify parent and caregiver training as a core component of any comprehensive ABA program.[3] What you do during bath time, breakfast, car rides, and bedtime is therapy. You just need the right framework to make it intentional.
ABS Includes Parent Training in Every ABA Program Because Sessions Alone Are Not Enough.
Fill in the form below to discuss how your child could start therapy quickly, without the stress:
6 ABA-Informed Parenting Strategies You Can Use at Home Starting Today
These are not simplifications. These are the actual techniques BCBAs teach in formal parent training sessions explained clearly enough that you can begin using them immediately.
Strategy 1: Antecedent Modification, Prevent Problems Before They Start
What it is: Antecedents are everything that happens before a behavior. If you can change the environment or the situation before a challenging behavior occurs, you prevent it rather than react to it.
How to use it at home: Before a transition your child struggles with (leaving the park, finishing screen time), give a 5-minute warning using a visual timer. Add a ‘first-then’ visual board ‘First shoes, then tablet.’ Remove the triggering demand from ambiguity by making what comes next predictable. Most meltdowns have a predictable antecedent, once you find it, you can modify it.
Strategy 2: Differential Reinforcement, Increase What You Want by Ignoring What You Don’t
What it is: Differential reinforcement means you reinforce the behavior you want while withholding attention from the behavior you don’t. It sounds simple but requires consistency to work.
How to use it at home: When your child asks for something appropriately, even a gesture, a look, a single word, respond immediately and enthusiastically. When they grab, scream, or drop to the floor for the same item, wait calmly for any approximation of appropriate requests before responding. The gap between how quickly you respond to each behavior is what drives the change. Track it for a week and you will see a pattern.
Read More: Understanding Hand Flapping in Autism
Strategy 3: Visual Schedules, Reduce Anxiety by Making the Day Predictable
What it is: Autistic children often experience significant anxiety from unpredictability. Visual schedules convert the invisible structure of the day into a concrete, scannable format the child can reference independently.
How to use it at home: Create a simple morning routine board using photos or picture icons, wake up, bathroom, get dressed, breakfast, school. Walk through it with your child every morning, having them physically move or flip each card as they complete it. Over time, the schedule reduces the need for verbal prompting because your child is orienting to the board rather than to you. This is an evidence-based antecedent strategy that generalizes to school immediately.
Strategy 4: Functional Communication Training, Respond to the Message, Not the Behavior
What it is: Most challenging behaviors in young autistic children are communication. The child does not yet have the words, signs, or symbols to express what they need, so they use the behavior they have.
How to use it at home: Before labeling a behavior as ‘defiant’ or ‘a tantrum,’ ask: what is this getting the child? Attention? Escape from a demand? A preferred item? Once you identify the function, teach a replacement, a word, a picture card, a gesture, that gets the same result. When the replacement works consistently and the challenging behavior stops working, the behavior decreases. This is FCT (Functional Communication Training), and parents can implement it at home with BCBA guidance.
Strategy 5: Errorless Teaching, Build Confidence by Making Success Inevitable
What it is: Traditional teaching lets children fail and then corrects them. Errorless teaching provides the correct prompt immediately before an error can occur, then gradually fades that support as the child masters the skill.
How to use it at home: When teaching your child to identify a color or complete a step in a routine, don’t wait for them to get it wrong. Say ‘point to the red one’ and physically guide their hand to the correct answer before they can hesitate. Reinforce immediately. Repeat. Gradually reduce the physical guidance over sessions. This builds fluency and confidence without the frustration cycles that come from repeated errors and corrections.
Strategy 6: Token Economy, Build Motivation for Harder Tasks
What it is: A token economy is a reinforcement system where the child earns tokens for specific behaviors and exchanges them for a preferred reward. It bridges the gap between a behavior and a reward that cannot be delivered immediately.
How to use it at home: Create a simple board with 5 spaces. Every time your child completes a difficult task, a transition, a demand, a social interaction, they earn a token (a sticker, a chip, a checkmark). When all 5 spaces are filled, they exchange the board for a preferred activity or item. The system makes the path to reinforcement visible and concrete, which dramatically reduces frustration during demanding tasks.
How Do You Know Which Strategy to Start With?
Start with the one that addresses your child’s most frequent and most disruptive challenge, not the most complex one. Use this as a guide:
If your biggest challenge is… | Start with this strategy | Why |
Meltdowns at predictable times (transitions, routines) | Antecedent Modification | Most meltdowns have a pattern. Changing what comes before is faster than managing the meltdown itself |
Challenging behaviors for attention or items | Differential Reinforcement + FCT | These work together, teach the replacement behavior while reinforcing it more than the challenging one |
Anxiety, rigidity, or resistance to change | Visual Schedules | Predictability reduces anxiety, the schedule does the work so your words don’t have to |
Reluctance to attempt new or hard tasks | Errorless Teaching | Errors breed avoidance. Remove the possibility of failure at first, then gradually fade support |
Short attention, difficulty completing multi-step tasks | Token Economy | Makes the abstract reward concrete and proximal, the child can see progress toward the goal |
Did You Know?
A 2022 study in the Journal of Autism and Developmental Disorders found that parents who completed structured ABA parent training reported significantly lower parenting stress scores after 12 weeks not just because their child’s behavior improved, but because the parents felt equipped to respond rather than reactively. Knowing what to do changes how the hard moments feel. [4]
3 Common Mistakes Parents Make When Implementing ABA Strategies at Home
- Inconsistency across caregivers: if one parent responds to grabbing and the other waits for appropriate requesting, the child learns to grab with the first parent. Both caregivers must respond the same way every time.
- Reinforcing too slowly: the window between a behavior and its reinforcement is seconds, not minutes. If the reward comes too late, the child cannot connect it to the right behavior. Reinforce immediately.
- Skipping parent training: attempting to implement ABA techniques without coaching from a BCBA often leads to inconsistent application that does not produce results and sometimes backfires. These strategies require supervision to get right. Ask your BCBA to walk through each one with you in a real session.
When Home Strategies Are Not Enough - Knowing When to Call a BCBA
These strategies are effective, but they are not a substitute for professional ABA programming when significant challenges are present. Seek an assessment from a BCBA if:
- Behaviors are unsafe: aggression, self-injury, elopement, or behaviors that put the child or others at risk require a formal Functional Behavior Assessment before any intervention is attempted
- Communication is significantly delayed: if your child has limited or no spoken language, a BCBA can assess AAC options (picture exchange, speech-generating devices) and design a communication program
- Home strategies are not working after 4–6 weeks: a BCBA can identify what is and is not working and adjust, most strategy failures are function mismatches, not approach failures
- Your child is approaching a major transition: school entry, a new sibling, a move, these are high-risk windows for behavioral regression that benefit from proactive BCBA support
At Achievement Behavior Services, parent training is built into every ABA program we design. Our BCBAs coach families in NY, NJ, CT, GA, and NC to implement these strategies in real time, not in a classroom, but in your kitchen, your car, and your morning routine. The goal is to make your whole day therapeutic, not just the hours a therapist is present.
ABS Parent Training Is Included in Every Program, In-Home and Center-Based Across 5 States.
Frequently Asked Questions — Autism Parenting Strategies
Q: What is the most effective parenting strategy for autistic children?
There is no single best strategy, it depends on the function of the behavior you are trying to change. That said, antecedent modification (changing the environment before problems occur) and functional communication training (teaching appropriate ways to express needs) produce the most consistent results across the most children. Both are well-supported in ABA research.[1]
Q: How do I stop my autistic child from having meltdowns?
Most meltdowns follow a predictable pattern, they have a consistent antecedent (trigger) and function (what they communicate). The fastest path to reducing meltdowns is identifying the trigger and modifying it before it escalates through visual schedules, advance warnings, and ‘first-then’ boards.[5] A BCBA can conduct a Functional Behavior Assessment to identify your child’s specific trigger chain if the pattern is not clear.
Q: Can parents do ABA therapy at home?
Parents can absolutely implement ABA-based strategies at home and research shows that parent-implemented ABA significantly improves outcomes.[2] However, parents should not design their own ABA program without BCBA guidance. A BCBA assesses the child, identifies strategy-behavior matches, and trains the parent on correct implementation. The parent then delivers the strategy; the BCBA supervises and adjusts. This combined model produces the strongest outcomes.
Q: What is parent training in ABA therapy?
ABA parent training is a structured process where a BCBA coaches caregivers to implement behavioral strategies, reinforcement, prompting, scheduling, and communication in the child’s natural environment.[3] It is not a class. It is hands-on coaching during real daily routines. The BACB identifies parent training as a required component of comprehensive ABA programming, not an optional add-on.
Q: How do I communicate better with my autistic child?
Three strategies make the biggest difference: use shorter, clearer instructions (one step at a time, not multi-part directions); add visual supports alongside verbal instructions (show and tell, not just tell); and wait longer after giving a prompt many autistic children need 5–10 seconds to process before responding, and interrupting that processing window restarts the clock.[6]
Q: What should I do immediately after my child receives an autism diagnosis?
Three immediate priorities: request a school evaluation in writing (this starts the IEP process under IDEA, at no cost to you); contact an ABA provider for an intake and waitlist placement (wait times can be several months); and begin parent training as early as possible while formal services are being arranged.[7] You do not need to wait for a formal ABA program to begin learning strategies that help your child today.
Q: How do I handle aggression in my autistic child?
Aggression in autistic children is almost always communicative, it is serving a function, most commonly escaping from demands, attention, or access to something desired. Do not attempt to manage aggression without first identifying its function through a Functional Behavior Assessment. Strategies applied to the wrong function often make aggression worse. If aggression creates safety risks, contact a BCBA immediately rather than waiting for a scheduled intake.
Q: How can I reduce my stress as an autism parent?
Research shows that parents who receive ABA training, not just their children, report significantly lower stress scores than those who do not.[5] Feeling equipped to respond, rather than reactive, is the primary driver of that reduction. Beyond training: build respite care into your weekly schedule (it is not optional for sustainability), connect with parent-to-parent support groups, and remember that your regulated nervous system is your child’s most important co-regulation tool. You cannot pour from an empty cup.
References
[1] Cooper JO, Heron TE, Heward WL. Applied Behavior Analysis (3rd ed.).
https://pmc.ncbi.nlm.nih.gov/articles/PMC2831449/
[2] Bearss K, Johnson C, Smith T, et al. Effect of Parent Training vs Parent Education on Behavioral Problems in Children With Autism Spectrum Disorder. JAMA.
https://pubmed.ncbi.nlm.nih.gov/25898050/
[3] Behavior Analyst Certification Board (BACB). Ethics Code for Behavior Analysts, Section 2.10 — Caregiver Training. Revised 2022.
https://www.bacb.com/ethics-information/ethics-codes/
[4] Minjarez MB, Williams SE, Mercier EM, Hardan AY. Pivotal Response Group Treatment Program for Parents of Children with Autism. Journal of Autism and Developmental Disorders.
https://experts.illinois.edu/en/publications/pivotal-response-group-treatment-program-for-parents-of-children-/
[5] Supekar K, et al. Impact of Early Intensive Behavioral Interventions on Young Children with ASD. PMC12514992. 2025.
https://pmc.ncbi.nlm.nih.gov/articles/PMC12514992/
[6] National Institute on Deafness and Other Communication Disorders (NIDCD). Autism Spectrum Disorder: Communication Problems in Children. Updated 2023.
https://www.nidcd.nih.gov/health/autism-spectrum-disorder-communication-problems-children
[7] U.S. Department of Education, OSEP. IDEA Part C: Early Intervention and Part B: IEP Rights for Children with Disabilities.
https://sites.ed.gov/idea/
[8] Dawson G, et al. Randomized Controlled Trial of Early Start Denver Model for Young Children with Autism — Parent Coaching Component. Pediatrics. 2010;125(1). PMC6034700.
https://pmc.ncbi.nlm.nih.gov/articles/PMC6034700/
[9] American Psychological Association (APA). Applied Behavior Analysis — Parent Training Overview.
https://www.apa.org/about/policy/applied-behavior-analysis
[10] Shaw KA, et al. Prevalence and Early Identification of ASD — ADDM Network, 2022. MMWR Surveillance Summaries. 2025;74(SS-2). CDC.
https://www.cdc.gov/mmwr/volumes/74/ss/pdfs/ss7402a1-H.pdf

